Sep 20th, 2021
HIV pre-exposure prophylaxis (PrEP) in Ontario, 2020
HIV pre-exposure prophylaxis (PrEP) is the use of daily antiretroviral medications by HIV-negative individuals to reduce their risk of HIV infection. PrEP is a highly effective HIV-risk reduction strategy and a critical part of a comprehensive approach to HIV prevention. To improve access to PrEP, it is important to monitor PrEP uptake. However, Ontario does not currently have a provincial-level monitoring system for PrEP.
To close this gap, the Ontario HIV Treatment Network is pleased to bring you this report summarizing PrEP uptake and PrEP prescribing in Ontario from 2016 to March 2020. This report contains projected provincial-level estimates which are based on Truvada (inclusive of generics) or Descovy dispensation data from more than 2,100 pharmacies across Ontario provided by IQVIA1. An update and expansion of the October 2019 PrEP report published by the OHTN (“HIV pre-exposure prophylaxis in Ontario”), this report describes:
- the estimated number, proportion or rate of individuals dispensed PrEP overall, by sex, age, prescriber specialty, payment type, region, and as a ratio to number of first-time HIV diagnoses (“PrEP-to-need ratio”).
- the estimated number, proportion or rate of physicians and nurse practitioners who prescribed PrEP overall, by sex, specialty, number of PrEP prescriptions written, region, and as a ratio to number of first-time HIV diagnoses (“PrEP prescriber-to-need ratio”).
The report also includes data on PrEP uptake among gay, bisexual, transgender, Two-Spirit, and queer (GBT2Q) men in Ontario from the 2019 Sex Now survey: an annual national online community survey of GBT2Q men’s health in Canada.
For more information about this report, email [email protected]. To learn more about PrEP, visit www.ontarioprep.ca. There you can learn more about PrEP and how to access PrEP regardless of drug coverage.
Some key findings
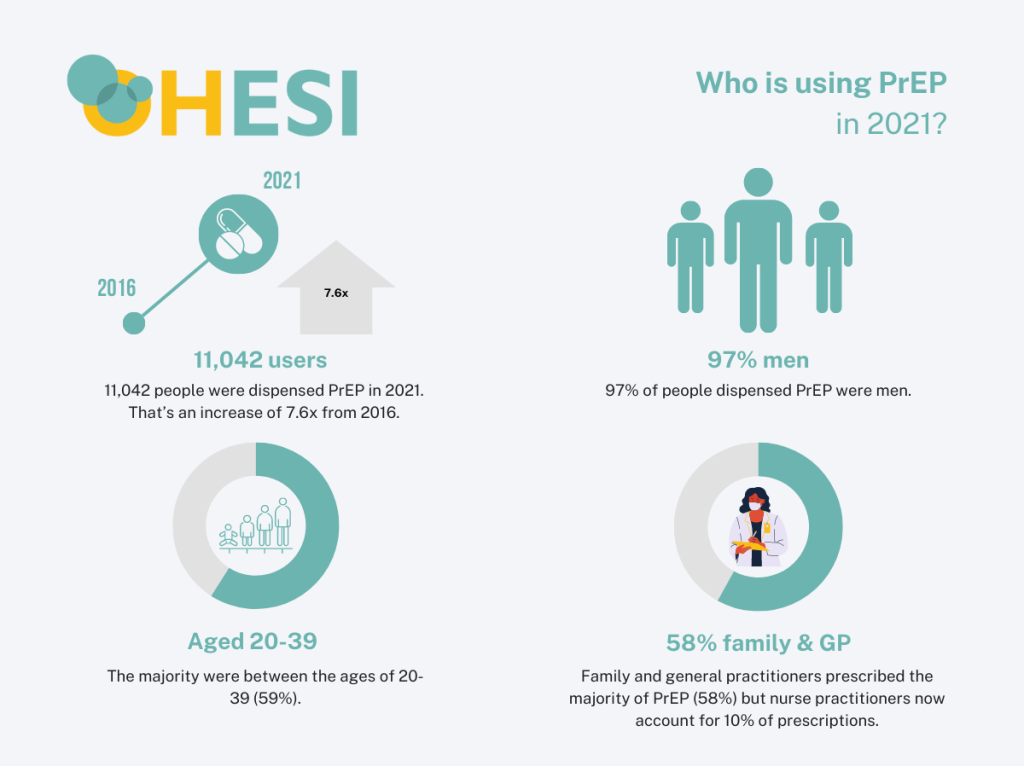
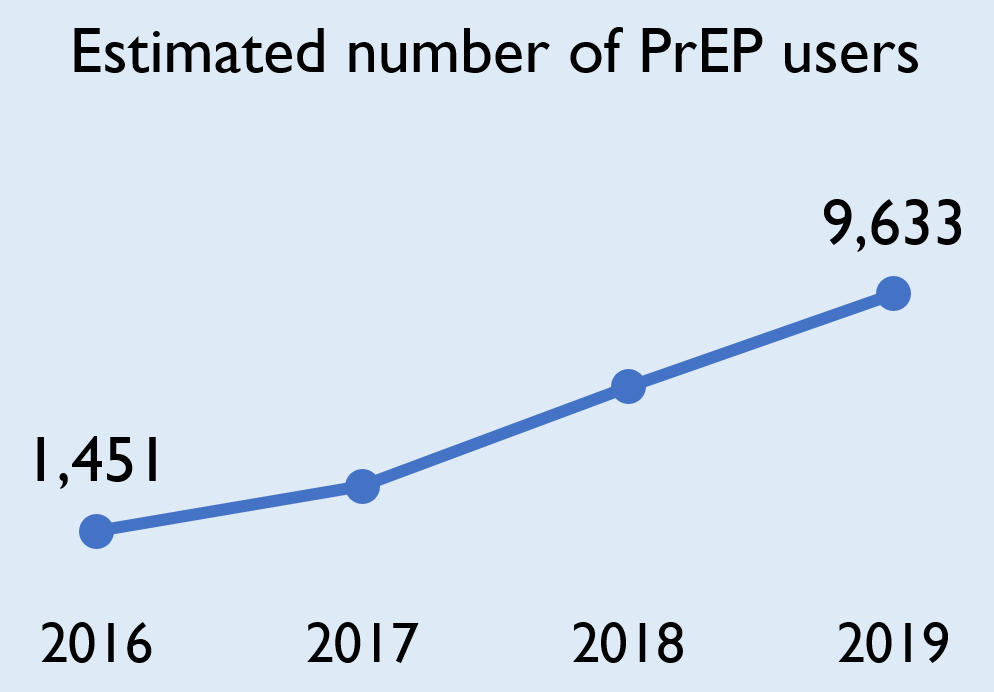
PrEP use is increasing
The estimated number of PrEP users in Ontario increased dramatically (6.6 times) between 2016 and 2019.

Most PrEP users are men
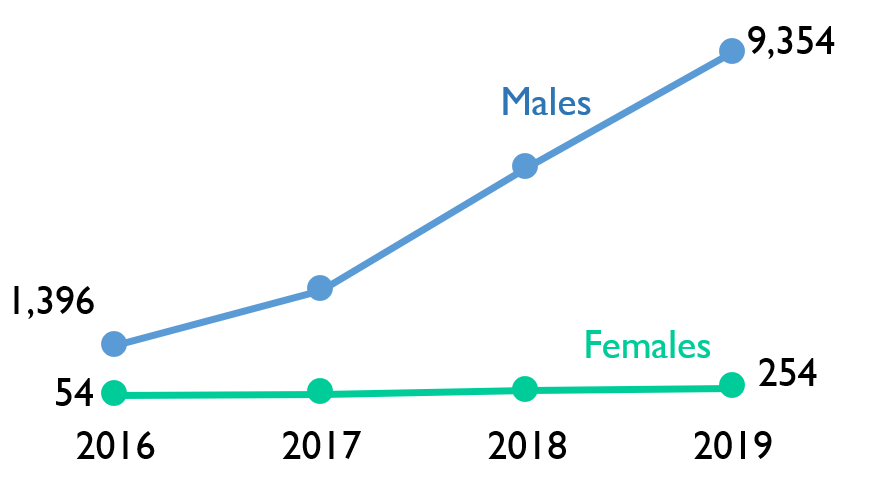
PrEP is indicated for gay, bisexual and other MSM who meet risk criteria. As we expect, the majority of PrEP users are male (97%). While, PrEP use has increased for both men and women, it is increasing faster for men.
Assessing successful uptake of PrEP in women is not straightforward, as overall risk for HIV in women is lower, and PrEP guidelines are less developed for women as compared to men.
Most PrEP users are people between the ages of 20 and 39
In 2019, 33% of PrEP users were aged 30-39 years and 26% of PrEP users were aged 20-29 years.

People mainly get PrEP from their family doctors and use private insurance to pay for it. In 2019…
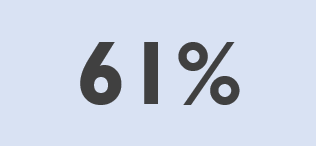
of the estimated PrEP users were prescribed PrEP by family and general practitioners.
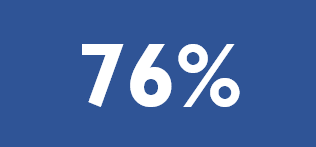
of the estimated PrEP users covered the cost of the prescription through private health insurance.
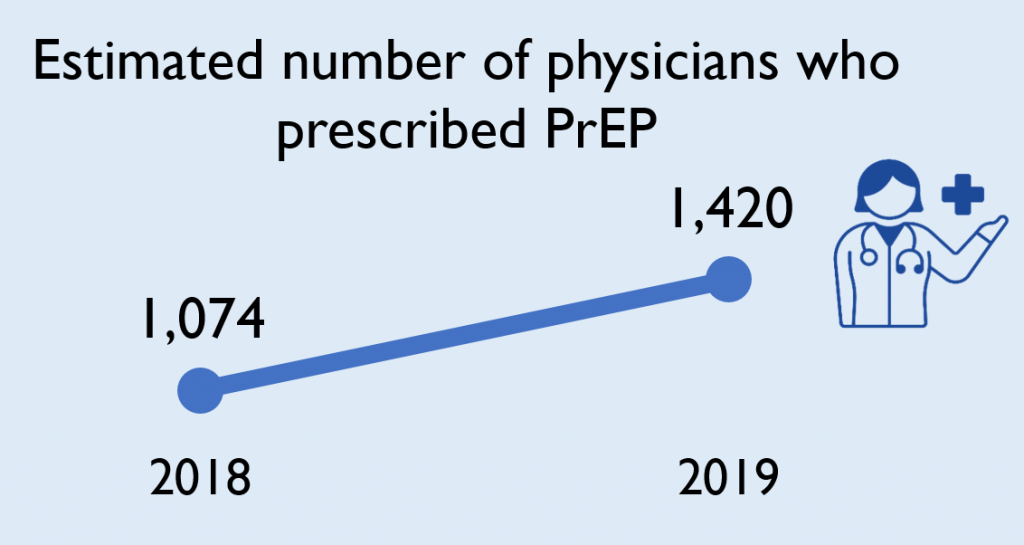
More physicians are prescribing PrEP
Between 2018 and 2019, the estimated number of physicians who prescribed PrEP increased by 32%.
Most PrEP prescribers are in Toronto and Ottawa
In 2019, Toronto and Ottawa had the largest number of physicians who prescribed PrEP – together accounting for 6 in 10 PrEP prescribers (60.7%) when these regions made up only 27.4% of Ontario’s population. This may be explained by Toronto and Ottawa having disproportionately more gay, bisexual, and other men who have sex with men (GBMSM) who are eligible for PrEP, and/or individuals traveling into these cities to obtain PrEP. Nevertheless, the number of PrEP prescribers increased between 2018 and 2019 for almost all regions in Ontario.
PrEP use is increasing for the people who need it the most
The PrEP-to-need ratio compares the number of PrEP users to the number of HIV diagnoses in a demographic group or geography. We use the PrEP-to-need ratio to determine whether groups with the greatest HIV burden are benefiting from the PrEP rollout. A higher ratio indicates that a group has greater PrEP coverage relative to its need.
Between 2016 and 2019, the PrEP-to-need ratio:
- increased for males and females.
- increased across all health regions and was highest in Ottawa in 2019.
- was higher for males than for females.

Assessing successful uptake of PrEP in women is not straightforward, as overall risk for HIV in women is lower, and PrEP guidelines are less developed for women as compared to men.
GBT2Q men who meet prescribing criteria are taking PrEP
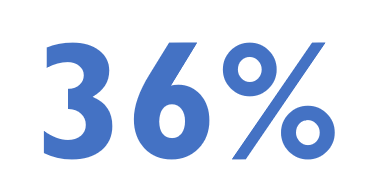
Among gay, bisexual, transgender, Two-Spirit and queer (GBT2Q) men in the Sex Now 2019 study who met the criteria for PrEP based on the Canadian guidelines, 36.0% were currently on PrEP.

Much more information is provided in the full report.
Footnotes
- IQVIA, formerly Quintiles and IMS Health, Inc., is an American multinational company serving the combined industries of health information technology and clinical research.